With recent government regulations affecting the healthcare industry, medically integrated and chiropractic practices have been impacted in numerous ways. Certain third-party health insurance payers have negotiated fee-for-service contracts with providers, which has resulted in lower reimbursement or no reimbursement, when it comes to the chiropractic office or a practice that has recently integrated.
The Healthcare Insurance Portability and Accountability Act, HIPAA, has also had an impact, by tightening the requirements for claim data submission, which can often be very difficult for the medically integrated practice and especially the chiropractic office, which already has limited access to third party payers, with added scrutiny. And as chiropractic or other healthcare practices transition to the medically integrated model (which includes, in addition to chiropractic, functional bracing, rehabilitation therapy, physical medicine and the systems related to successfully operating a medically integrated practice), these practices and providers have had to adjust the way they bill for care provided.
Due to these changes in their model and government regulations, having a healthy revenue cycle is more important than ever and is often a new subject for the newly medically integrated medical private practice or chiropractic office.

What is the Integrated Medical Office Revenue Cycle?
What exactly does the term “revenue cycle” mean in relation to a private medically integrated practice? The revenue cycle is defined as all administrative and clinical functions that contribute to the capture, management, and collection of patient service revenue. In the most simplistic and basic terms, this is the entire life of a patient account from creation to payment.
For a chiropractic office that has transitioned into the new medically integrated model, this may be something very new or significantly expanded.
A healthy revenue cycle should follow billing and collection best practices to ensure that cash is properly collected for cash-services, bills are submitted in accordance with payor requirements and all services provided are billed and/or collected. The last thing that a medically integrated practice needs is to provide services and not be paid.
Integrated Practice Revenue Cycle Leakage Points
There are many different leakage points in the revenue cycle, but here are the most common:
- Not collecting for cash-only services at time of service
- Registration, coding or billing errors for expanded services
- Unverified insurance
- Underpaid claims
- Denied claims
- Denied appeals
Knowing the right systems and working with the right group, such as Advanced Medical Integration, to implement them is very important in preventing these leakage points.
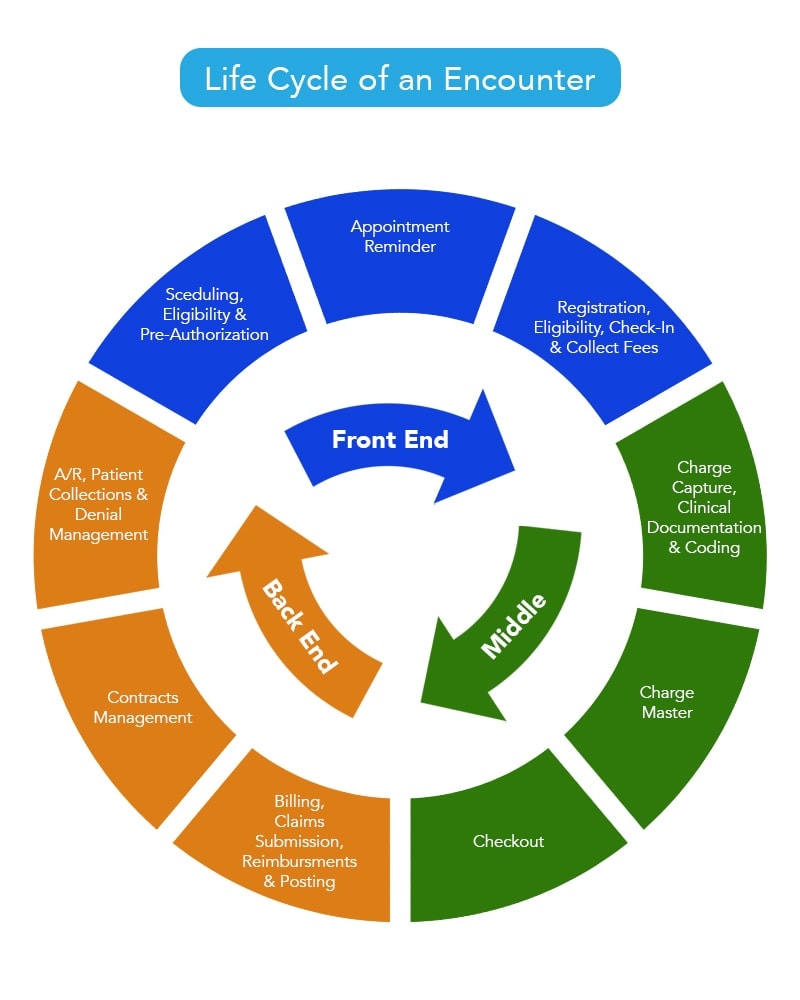
Medically Integrated Practice Professional Billing and Collection Best Practices
There are various best practices and systems your medically integrated practice should incorporate for a healthy revenue cycle. Some of these you’re already doing and some will be new.
Some of the best practices include:
- Proper Credentialing – If you are in network, proper credentially in necessary. Credentialing is the process of obtaining, verifying, and assessing the qualifications of a practitioner to provide care or services in or for a healthcare organization. Credentials are documented evidence of licensure, education, training, experience, or other qualifications.
- Define cash-only services – In an integrated medical model there are services, such as natural medicine, that is cash-only service. Educating your patients on what services are included in this payment method and when payment is expected is a key part of proper collections. This should include education on cost saving incentives that patients can take advantage of as well.
- Conduct Financial Clearance – This includes maintaining and verifying patient information before the patient arrives for their appointment. Insurance eligibility is checked and authorizations are tracked. Patients are notified of outstanding balances and prompt payment is encouraged.
- Streamlined Check-In & Check-Out Process – Patient information is confirmed and verified, eligibility determination is conducted; prior and new balances are collected.
- Charge Capture – An electronic charge capture process is utilized; specific coding situations are managed; documentation audits are performed.
- Charge Entry – During this phase, fee schedules are developed and managed; charges are entered; charges are reviewed and audited; the person responsible for editing charges is strictly controlled.
- Proper Documentation – Ensuring that patient records from intake, history of ADL’s, exam, report of findings, care plans, soap notes, re-exam notes, new orders, additional soap notes and discharge documentation are all properly completed and and managed.
- Proper Claims Management – Electronic claims are submitted and status updates are frequent; secondary claim process happens; attention is paid to maintain compliance with insurance carrier’s claim format requirements; there are multi-tiered claim editing checks; assistance with edit tracking and error resolution happens; a system for easy rebilling or corrected claim processing is implemented; and an overall analysis of billing process delay times is taking place.
- Patient Statements – In the patient statements phase, cycled billing occurs; statements are clear and concise; there are notes and automated holds on patient statements when applicable; final notices go out.
- Payment & Denial Posting – This phase includes the entering of payments; the managing of contractual write-offs; the processing of insurance reversals; credit balance resolution; the review of denials and adjustments; and the control of who can edit payments.
- Insurance Follow Up – Verification that insurance carriers are receiving claims and that the claims are being processed; accounts receivable are worked on by priority; staff’s collection actions are audited; your practice’s average days in accounts receivable and net collection rates are known.
- Denial Management – During denial management, you’ll know if your claims denials rate is excessive; there is understanding of the claims denials received; your common denial causes are analyzed to improve processes; and denied claims are resubmitted if payment can still be collected.
- Patient Collections – During the patient collections phase, patient billing occurs; collection letters are sent; general collections take place; payment plans are offered; patient balances are reviewed before appointments; the productivity of collectors is analyzed. If the earlier steps are properly executed, patient collections should run smoothly and with minimal patient frustrations.
- Payor Management – In this phase, attention is paid to fee schedules, carrier provider numbers and NPI, assignment of benefits, carrier communications and contract dates, documentation to support claims, and carrier analysis take place.
Advanced Medical Integration (AMI) is the nation’s leading consulting group for establishing a holistic, philosophically-based medically integrated practice. Whether you are new to medical integration or already have an integrated clinic, AMI will help you develop your practice to the new standard in desired holistic medical services.
Chiropractors, are you looking for answers? CLICK HERE or follow AMI on YouTube to find out how our approach is helping practice owners like you recover their customers and grow. We’ll work with you to open up new opportunities for your patients, your practice, and YOU!
Call 1-888-777-0815 for more information today!


